Important aspects about treatment with platelets – PRP
Platelets are biological components of the blood, along with red and white blood cells. Unlike red and white blood cells, platelets do not have a nucleus and, therefore, do not qualify to be called “cells.” They are slightly smaller than red and white blood cells.
Platelets are probably best known as components of the blood coagulation system. When an injury breaks a blood vessel and causes bleeding, platelets quickly come into action to contribute, along with fibrin, to the formation of a clot. However, platelets are more than just the first line of response to a bleeding wound. Each platelet is also a biochemical source of signaling molecules (bioactive proteins) that participate in tissue regeneration, healing, and the emergency response to injuries.
Among these molecules are Platelet-Derived Growth Factors, which can activate Peripheral Stem Cells to fulfill these functions.
- Main growth factors associated with platelets:
- What is PRP (Platelet Rich Plasma)?
- How is PRP obtained?
- PRP in hair transplant.
- To preserve and improve the viability of the grafts.
- To promote and improve tissue repair and healing.
- To revitalize inactive follicles by stimulating the growth and thickness of existing miniaturized hair or transplanted hair.
Main growth factors associated with platelets:
– Platelet-Derived Growth Factor (PDGF): Promotes the growth of blood vessels, cell replication, and skin formation.
– Transforming Growth Factor-beta (TGF-β): Promotes the growth of the matrix between cells and bone metabolism.
– Vascular Endothelial Growth Factor (VEGF): Promotes the formation of blood vessels.
– Epidermal Growth Factor (EGF): Promotes cell growth and differentiation, blood vessel formation, and collagen formation.
– Fibroblast Growth Factor (FGF): Promotes the growth of specialized cells and the formation of blood vessels.
– Insulin-Like Growth Factor (IGF): It is a regulator of physiological processes in almost all cells of the body.
– Platelet-Derived Growth Factor (PDGF): Promotes the growth of blood vessels, cell replication, and skin formation.
– Transforming Growth Factor-beta (TGF-β): Promotes the growth of the matrix between cells and bone metabolism.
– Vascular Endothelial Growth Factor (VEGF): Promotes the formation of blood vessels.
– Epidermal Growth Factor (EGF): Promotes cell growth and differentiation, blood vessel formation, and collagen formation.
– Fibroblast Growth Factor (FGF): Promotes the growth of specialized cells and the formation of blood vessels.
– Insulin-like Growth Factor (IGF): Regulator of physiological processes in almost every cell of the body.

All these growth factors at work enhance physiological processes that contribute to tissue recovery after an injury. Growth factors are also involved in the formation of new blood vessels.
The rationale for using PRP in surgery is to artificially increase the number of platelets at a site where the reservoir of growth factors is located, serving to improve tissue recovery, repair, and health.
What is PRP (Platelet Rich Plasma)?
It is a platelet concentrate obtained from the patient’s own plasma, containing significant reserves of growth factors and peripheral stem cells that are crucial for initiating and accelerating tissue repair and regeneration. PRP is “autologous,” meaning it does not elicit an allergic response, is immunologically neutral, and carries no risk of disease transmission. PRP has been successfully used in neurosurgery, ophthalmology, urology, cardiac surgery, thoracic surgery, maxillofacial surgery, dentistry, and cosmetic surgery.

How is PRP obtained?
It is obtained through a simple venous blood extraction from the patient, similar to what is done for a laboratory test. This blood is centrifuged and processed to obtain a fraction that contains 4 to 8 times more platelets per cubic centimeter than normal plasma.
PRP in hair transplant.
The potential for using PRP to promote healing and hair growth after transplantation focuses on three functional applications:
– To preserve and enhance the viability of grafts during and after hair transplantation.
– To promote and improve tissue repair and healing after hair transplantation.
– To revitalize inactive follicles and stimulate the growth of new hair.
To preserve and improve the viability of the grafts.
From the moment hair follicles are harvested from the donor area of the scalp and transplanted to the recipient area, they are subjected to damage caused by various factors:
– Dehydration if the donor follicles are not adequately moistened between extraction and transplantation.
– Lack of oxygen and nutrients, as the blood supply is cut off upon separation from the body.
– Changes in temperature and pH in the follicle’s environment.
– Revascularization of grafts in the recipient area, upon which they depend to receive a new blood supply as soon as possible.
To maintain the viability of grafts during the transition period from extraction to placement, a storage solution is used that provides a protective environment, adequate moisture, proper temperature, chemical balance, and nutrient supply. Recent studies have indicated that the addition of PRP to this storage solution improves the viability of the follicle during and after transplantation, accelerates tissue healing, and promotes hair growth after transplantation. An approach advocated by some researchers is to bathe the grafts in PRP just before they are placed.
To promote and improve tissue repair and healing.
Individual growth factors such as PDGF have been used by surgeons to promote wound healing in hospitalized surgical patients. The justification for using PRP in outpatient hair restoration surgery is to utilize the full range of platelet growth factors to promote healing and minimize scarring, as well as to stimulate hair growth in transplanted follicles.
One method involves applying PRP to the micro-incisions on the scalp that will host the grafts, or injecting a PRP gel into the wound of a strip at the time of closure. It can also accelerate and improve the healing of the micro-wounds resulting from an FUE procedure.
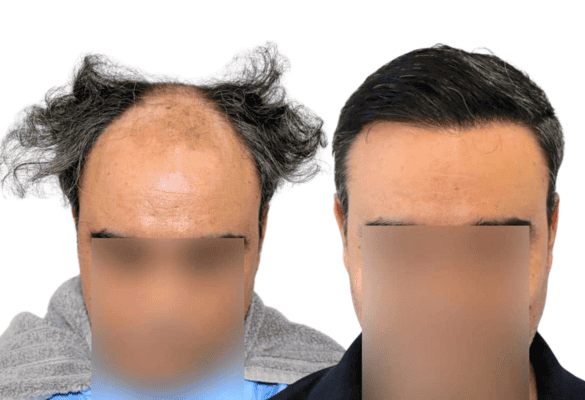
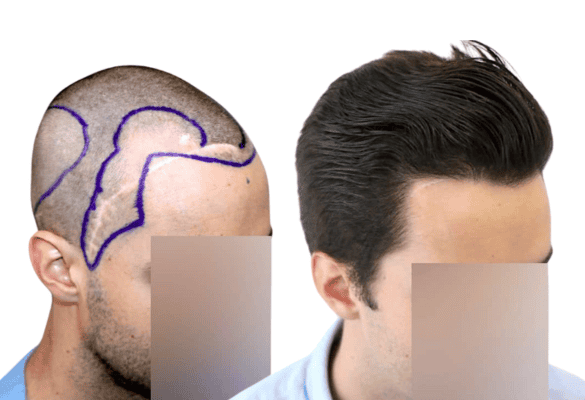
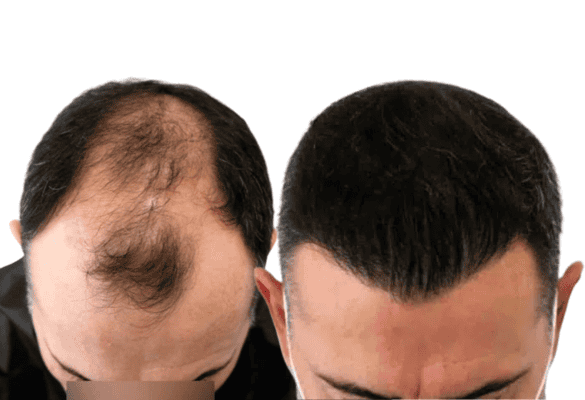
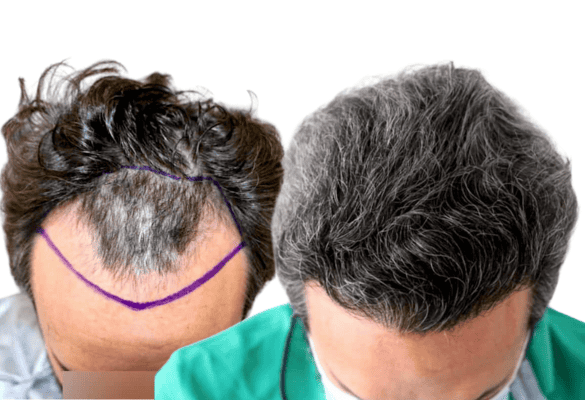
To revitalize inactive follicles by stimulating the growth and thickness of existing miniaturized hair or transplanted hair.
The follicles that are in the resting phase (telogen) can transition to the growth phase (anagen) stimulated by this treatment.
Improvement in hair growth, diameter, and the cessation of hair loss has been observed after 4 months of treatment. This use of PRP is still considered experimental and requires additional studies with positive statistics for scientific consideration.